A novel topical application influences closure of plantar ulcers in leprosy patients: Case studies in India.
Reynolds, C. L., Reynolds, S. J., Vardharajan, J. L.Sci. Healing Outcomes. 2014. Vol. 6. No. 22. 11-17 (Complete article)
Abstract
Objective: To determine the effect of a topical wheatgrass application on closure of chronic leprosy-related plantar ulcers.
Methods: patients undergoing longstanding leprosy treatment who also had plantar ulceration were enrolled. A topical spray was applied on alternate days. Serial pre- and post-treatment photographs were compared over 12 months to assess the degree of ulcer closure.
Results: Of the 21 patients enrolled, 19 patients suffering from 28 plantar ulcers completed the study. Application of a topical wheatgrass extract spray led to complete or significant closure of the leprous lesion in the majority of participants. Eleven of 28 ulcers (39%) experienced 100% wound closure. A clear, staged pattern of healing also emerged.
Conclusions: Based on these case studies, a topical spray derived from wheatgrass sprout extract shows promise as a healing agent for leprous ulcers.
Running Head: Topical application on leprous ulcers.
Keywords: Wheatgrass, trophic ulcer, topical, leprosy, wound healing.Signed patient consent forms are available on request.
Introduction
Although cure rates for leprosy are high in individuals undergoing multiple drug therapy, between 10 to 20% of patients are left with trophic plantar ulcers.1 Trophic ulcers are typically chronic and slow to heal; they may persist for years or in some cases for the life of the patient. These ulcers are associated with tissue loss, decreased or absent sensation, decreased blood supply, and underlying osteomyelitis. Many patients lose the ability to perform normal daily activities2. Further more, leprous ulcers may lead to social stigma and ostracism that persists to this day3.
Many remedies have been trialled to encourage healing of leprous ulcers, but with limited success4-7. Surgical intervention may be effective in some patients1,8. Walking casts and properly designed footwear can be effective in limiting further damage, but do little to promote healing. A number of pharmaceutical products such as topical phenytoin have been trialled, but tend to be expensive and of limited value 9. Currently there is no simple, inexpensive, treatment that actively promotes leprous ulcer healing.
Wheatgrass and other cereal grasses have been used as healing remedies for millennia. In the mid-1930s and 1940s, cereal grass extracts became the focus of clinical and laboratory studies in the United States. These extracts were able to heal suppurative and non-suppurative wounds10-14 . This pilot case series was conducted to assess the effect of a topical wheatgrass extract spray on longstanding leprous plantar ulcers. In a small patient population, the spray helped promote re-vascularization, ulcer healing, and wound closure in the majority of patients.
Materials and Methods
Patient selection
Study participants were recruited from two Indian cities, Indore and Khandwa, in Madhya Pradesh Province, India. Patients included in the study were over 17 years of age, carried a diagnosis of multibacillary or paucibacillary leprosy, and had one or more plantar ulcers of at least six months duration. Patients were excluded if they could not read and sign an informed consent document. All patients were receiving dapsone, clofazamine and rifamycin for a year or more prior to the study. All participants continued oral leprosy treatment during the study.
Treatment Administration and Data Collection
A commercially produced 4% wheatgrass extract solution, (Dr. Wheatgrass Skin Recovery Spray, Wheatgrass Pty. Ltd., Australia) was sprayed on the ulcer surface every second day and a light dressing applied. Photographs were obtained for assessment and comparison over a 12 month period. Percentage of closure was measured directly from the photographs or the ulcer declared “healed.”
Patient details included leprosy classification (WHO)15, age, gender, ulcer location, current medication, other medical conditions and the duration of ulcer(s) under study. Estimated ulcer duration was based on patient recall at the time of enrolment. Informed consent was obtained through written medical release forms prior to treatment.
Results
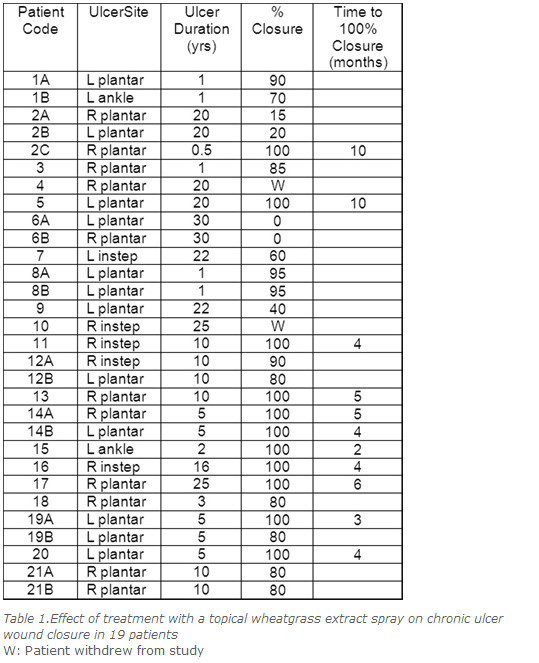
Twenty-one patients suffering from 30 trophic plantar ulcers were included in the study. Two participants were excluded from further analysis because one required pedal amputation (Patient 4) and the other did not adhere to treatment (Patient 10) leaving 19 patients with 28 ulcers. Of these patients, 10 (53%) were male. Most patients were elderly with a mean ± SD age of 57.9 ± 8.8 years. The age range was 40 to 75 years (female mean = 59.5, male mean = 56.2). Patients had leprosy for 10 to 50 years (mean 30.5 years). Most patients (90%) had multibacillary leprosy as defined by the WHO15 while the remaining two patients had paucibacillary leprosy. Two patients had type 2 diabetes mellitus (Patients 1 and 21).
The topical spray was tested in trophic ulcers of the lower leg and foot exclusively. Most ulcers were located on the foot (Table 1). Patients had suffered from their ulcers for an average of 10.4years prior to entering the study (range six months to 30 years).
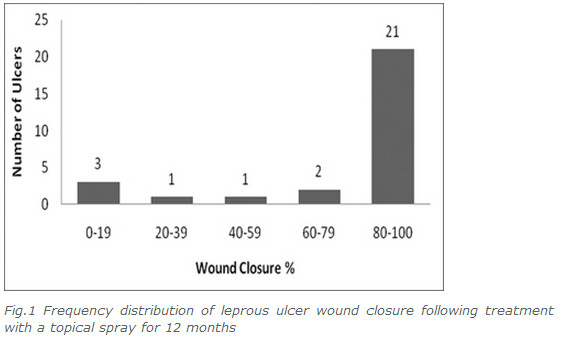
After topical treatment all ulcers displayed signs of healing including revascularisation, self-debridement and re-filling. Three-quarters of treated ulcers (21 out of 28) demonstrated at least 80% closure following treatment (Figure 1). Eleven of 28 ulcers (39%) experienced 100% wound closure.
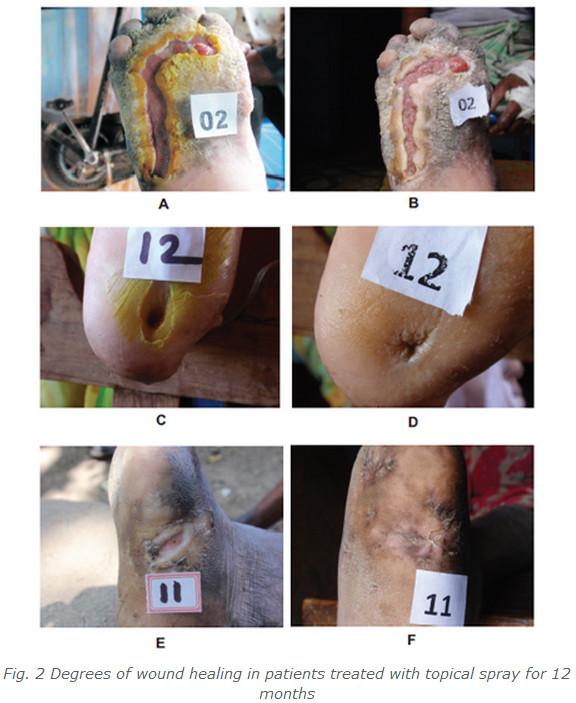
Images of lesions prior to treatment are shown for patients 12, and 11 (Panels A, C, and E respectively)in Figure 2. Panel B shows an example of 15% wound closure, Panel D shows 80%, and Panel F shows 100% closure.
Two ulcers occurring in the same patient, while improved in appearance and degree of debridement, did not reduce in size appreciably (Ulcers 6A and 6B). Pain sensation in the affected area returned in two patients (Patient 2/Ulcer 2A and Patient 21/Ulcer 21A).
Discussion
The topical application of a wheatgrass extract spray led to trophic ulcer healing in most patients in this case series. This result was surprising given the age of many of the ulcers treated. A number of topically applied treatments have been studied including phenytoin4 , metronidazole1 7 , thalidomide18, radiation-processed amniotic membranes7, ketanserin19, and sulphadiazine20 cream. Based on the results of our case series, a topical spray containing wheatgrass extract appears to be as or more effective than these interventions. While it may be less expensive and resource intensive than surgery or specialized footwear, drug therapy still may be financially prohibitive for people in developing nations. In fact, the cost-effectiveness of current interventions to treat leprous ulcers has been questioned21. One inexpensive treatment, 3% citric acid, exhibited healing effects similar to the spray used in this study, but this has only been demonstrated in one patient to date22.
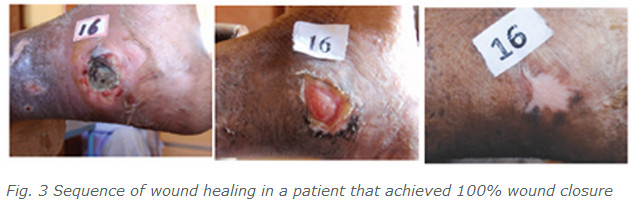
With topical wheatgrass extract spray treatment, most leprous ulcers followed a predictable pattern of healing (Figure 3). Revascularization occurred first, usually within the first two weeks; this involved healthy revitalization of the ulcer floor evidenced by increased exudate and colour change from pallid brown to reddish pink. Over the next several months, most ulcers “enlarged” as debridement of callus overriding the wound occurred. Granulation, filling, and wound closure occurred in most patients. While most epithelialisation advanced from the edges of the ulcer, in some cases islands of healthy skin emerged on the ulcer surface and fused with the advancing edge.
During our study, patients did not receive special footwear and continued to ambulate. Previous work in this area has suggested that reduced workload and avoidance of long distance walking are key interventions in trophic ulcer treatment.16 Our findings suggest that patients that continue to walk during healing may be helped by topical medications. Indeed, topical treatment with wheatgrass extract may accentuate or improve upon existing ulcer interventions such as surgery or specialized footwear.
Wheatgrass has been used as a medicinal agent in some countries for millennia but has not been evaluated clinically commensurate with this use. Grass extracts were the focus of research prior to 1950 as they were found to have growth stimulating properties11,12,13,23 and chlorophyllin (a mixture of various cereal grass extracts and a food colourant), was used to heal suppurative and non-suppurative wounds and was widely researched in large teaching hospitals10-12. Clinical and scientific observation suggests wheatgrass and other cereal grasses contain growth and fertility factors23 that facilitate the healing process of open wounds, ulcers and refractory skin grafts. The healing process may be augmented by the agent's antibacterial properties24,25. Considerable evidence points to the ability of cereal grasses to influence gene expression, particularly in diseased cells26-27.
One of the most peculiar findings in this case series was return of pain sensation in aged leprous ulcers. Leprosy affects the nerves supplying the skin's micro circulation. Restored sensation may suggest re-establishment of the microvascular circulation and the regeneration of peripheral nerve endings.
The current study is limited by the absence of a placebo comparator arm and is presented as a case series. It should be noted that while patients were receiving ongoing multi drug leprosy treatment during the study, this treatment commenced a year or more before wheatgrass extract treatment was initiated. In most cases oral leprosy treatment predated this study by several years. Therefore it is unlikely that plantar ulcer healing would have occurred spontaneously in this cohort given the chronicity of the ulcers and leprosy treatment. Likewise, it is unlikely that simple light wound dressings would be responsible for such rapid and profound healing.
In summary, wheatgrass extract appears to be an effective treatment for plantar ulcers resulting from leprosy. Given its low cost, wheatgrass extract may be especially attractive for use in poor countries where leprosy is endemic. The results of this study warrant an investigation of topical wheatgrass extract spray in a larger, placebo-controlled trial, and research into the mechanisms underlying its physiological effects.
Acknowledgements
The funding and wheatgrass extract, namely Dr Wheatgrass Skin Recovery Spray used for this study was provided by Wheatgrass Pty. Ltd. Queensland, Australia.
Conflict of interest: The project has been supported by the company that manufactured the product used in the study i.e. an extract of wheatgrass sprouts.
References:
- Bhatt YC, Panse NS, Vyas KA, Patel GA. Free tissue transfer for trophic ulcer complicating leprosy. Indian J. Plast. Surg.2009; 42: 115-117.
- Van Brakel WH. Peripheral neuropathy in leprosy and its consequences. Lepr. Rev.2000; 71 Suppl: S146-153.
- Van Brakel WH, Sihombing B, Djarir H, et al. Disability in people affected by leprosy: the role of impairment, activity, social participation, stigma and discrimination. Glob. Health Action.2012;5.
- Bansal NK, Mukul. Comparison of topical phenytoin with normal saline in the treatment of chronic trophic ulcers in leprosy. Int. J. Dermatol.1993; 32: 210-213.
- Bauman JH, Girling JP, Brand PW. Plantar pressures and trophic ulceration. An evaluation of footwear. J. Bone Joint Surg. Br.1963; 45: 652-673.
- Kaada B, Emru M. Promoted healing of leprous ulcers by transcutaneous nerve stimulation. Acupunct. Electrother. Res.1988; 13: 165-176.
- Singh R, Chouhan US, Purohit S,. Radiation processed amniotic membranes in the treatment of non-healing ulcers of different etiologies. Cell Tissue Bank.2004; 5: 129-134.
- Gravem PE. Heel ulcer in leprosy treated with fasciocutaneous island flap from the instep of the sole. Scand. J. Plast. Reconstr. Surg. Hand Surg.1991; 25: 155-
160. - Forsetlund L, Reinar LM. Quality of reporting and of methodology of studies on interventions for trophic ulcers in leprosy: a systematic review. Indian J. Dermatol. Venereol. Leprol. 2008; 74: 331-337.
- Carpenter EB. Clinical experiences with chlorophyll preparations with particular reference to chronic osteomyelitis and chronic ulcers. Am. J. Surg.1949; 77: 167-171.
- Chernomorsky SA., Segelman AB. Biological activities of chlorophyll derivatives. N. J. Med.1988; 85: 669-673.
- Gruskin B. Chlorophyll—Its therapeutic place in acute and suppurative disease: Preliminary report of clinical use and rationale. Am. J. Surg.1940; 49: 49-55.
- Gahan E, Kline PR, Finkle TH. Chlorophyll in the treatment of ulcers. Arch. Dermatol. 1943; 47: 849-851.
- Reynolds CL. The demise of chlorophyll and a fresh look at wheatgrass therapy. J. Australasian Integr. Med. Assoc.2004.
- World Health Organization. Guide to elimination of leprosy as a public health problem. Geneva 2000.
- Yan L, Zhang G, Zheng Z, et al. Comprehensive treatment of complicated plantar ulcers in leprosy. Chin. Med. J. (Engl).2003; 116: 1946-1948.
- Mishra S, Singh PC, Mishra M. Metronidazole in management of trophic ulcers in leprosy. Indian J. Dermatol. Venereol. Leprol.1995; 61: 19-20.
- Perri AJ, Hsu S. A review of thalidomide's history and current dermatological applications. Dermatol. Online J.2003; 9: 5.
- Salazar JJ, Serrano GG, Leon-Quintero GI, Torres-Mendoza BM. Use of topical ketanserin for the treatment of ulcers in leprosy patients. Indian J. Lepr. 2001; 73: 103-110.
- Bedi BM. Topical sulphadiazine cream for plantar ulcers. Indian J Lepr.1990; 62: 158.
- van Veen NH, McNamee P, Richardus JH, Smith WC. Cost-effectiveness of interventions to prevent disability in leprosy: a systematic review. PLoS One.2009; 4: e4548.
- Nagoba BS, Wadher BJ, Chandorkar AG. Citric acid treatment of non-healing ulcers in leprosy patients. Br. J. Dermatol.2002; 146: 1101.
- Kohler GO, Elvehjem CA, Hart EB. Growth stimulating properties of grass juice. Science.1936; 83: 445.
- Young RW, Beregi JS, Jr. Use of chlorophyllin in the care of geriatric patients. J. Am. Geriatr. Soc.1980; 28: 46-47.
- Johnson HM. Dermatologic evaluation of yeast, tyrothricin, chlorophyll and nitrofurazone. Arch. Derm. Syphilol.1948; 57: 348-356.
- Reynolds C. A DNA-technology-based cellular assay used to measure specific biological activity in a wheatgrass extract. J.Australasian Integr. Med. Assoc. March 2006.
- Okai Y, Higashi-Okai K, Yano Y, Otani S. Suppressive effects of chlorophyllin on mutagen-induced umu C gene expression in Salmonella typhimurium (TA 1535/pSK 1002) and tumor promoter-dependent ornithine decarboxylase induction in BALB/c 3T3 fibroblast cells. Mutat. Res. 1996 Aug;370(1):11-7.C. L. Reynolds,
S. J. Reynolds.
L. Vardharajan.
Correspondence: Dr. C. Reynolds: info@wheatgrasshealing.info